Images Reveal Potential for NIR Imaging to Detect Success of Breast Reconstruction
Submitted by ianm on 25 September 2012 - 2:54pm
In 2010 breast reconstruction entered the Top Five list of reconstructive procedures in the US, with 93,000 procedures performed, up 8% from 2009, and 18% from 2000. This is among the most common skin flap procedure performed.
Skin flaps are typically used to cover areas of tissue loss or defects that arise as a result of traumatic injury, reconstruction after cancer excision and repair of congenital defects. In the case of a mastectomy—the surgical removal of the breast—skin flaps are commonly used to create a new breast. Most commonly these flaps are derived from the woman’s own abdominal tissue, which is removed and transplanted to the breast area where it is formed to take on the shape and appearance of an actual breast (this is called the flap).
Skin flaps are complex procedures that require post-operative monitoring to ensure that they do not fail. Most failures arise from circulatory complications where either the arterial blood supply to the flap is blocked or insufficient to support the flap tissue or venous drainage of the flap is compromised.
Near infrared (NIR) spectral imaging is a convenient, non-invasive method for surgeons to examine flaps during surgery and in the early post-operative period. The NIR technique can be used to detect and localise blood supply-related complications as well as give real-time feedback to the surgeon as they try to resolve the complication.
In a paper* published in JNIRS—Journal of Near Infrared Spectroscopy, Dr Mike Sowa and his team at the National Research Council Canada report pre-clinical results showing the potential of NIR spectral imaging for intra-operative skin flap assessment.
“We also show that using estimates of tissue haemoglobin oxygen saturation, imaging measurements made during surgery and in the early post-operative period are highly predictive of the outcome of the flap tissue with specificities and sensitivities exceeding 85%”, Dr Sowa stated.
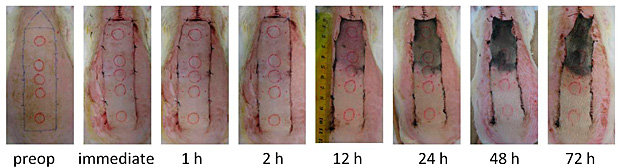
Oxygenation imaging immediately after surgery shows good predictive power for tissue necrosis. The prediction accuracy of the oxygen saturation parameter improves as measurements are made later in the post-operative period and becomes an excellent predictor of outcome when measurements are made one or two hours after the surgery. This method is highly capable of predicting the fate of flap tissues.
Dr Sowa’s paper is just one of 11 papers in the current, special issue of JNIRS—Journal of Near Infrared Spectroscopy dedicated to NIR imaging. The issue is essential reading for anyone who needs a picture of what is inside something without destroying it.
Guest Editor of the special issue, Professor Marena Manley, said the advantages of NIR imaging are substantial and include low cost analysis per sample, more rapid analysis and the ability to operate in a number of in-field or on-line/at-line environments; hence leading to savings in laboratory cost and gains in product value.
*The research is published as Michael G. Sowa, Jeri R. Friesen, Michelle Levasseur, Bernhard Schattka, Leif Sigurdson and Thomas Hayakawa, “The utility of near infrared imaging in intra-operative prediction of flap outcome: a reverse McFarlane skin flap model study”, J. Near Infrared Spectrosc. 20(5), 601–615 (2012), doi: 10.1255/jnirs.1007